Pregnancy Risks of Reversing Essure
Essure removal With Dr Monteith: Analysis of 469 Patients
The risks of reversing Essure are not limited to surgery, but also include pregnancy risks of reversing Essure.
In January of 2018, Dr. Monteith performed an analysis on the risks of reversing Essure and the risk of removing Essure devices at A Personal Choice.
From January of 2009 to January of 2018, Dr. Monteith performed 469 surgeries to remove Essure sterilization devices.
The following pregnancy complications were observed in the group of 469 patients who had Essure removal with Dr. Monteith.
Pregnancy Risks of Reversing Essure
- Closure of the tubes after reversal <60%
- Ectopic (tubal) pregnancy 5%
- Uterine rupture 4%
Closure of the fallopian tubes after Essure reversal

Essure Reversal Monteith Miracle Baby
Although closure of the tubes is not exactly a pregnancy complication, closure of the tubes after reversal of Essure is possible and may make natural conception more difficult.
Essure sterilization is the most difficult type of tubal ligation procedure to reverse.
The fallopian tubes are delicate and shaped like a funnel. The widest part of the fallopian tube is near the ovary. The narrowest part of the fallopian tube is near the uterus and has to travel through the thick uterine muscle. This is the location where the fallopian tube must be repaired during Essure reversal.
Since reversing Essure requires implanting (tubouterine implantation) the narrowest portion of the fallopian tube through the thickest part of the uterine muscle this area may be more prone to healing closed with scar tissue.
It is difficult to determine the exact chance of closure of the fallopian tubes after surgically reversing Essure sterilization.
We estimate the chance of tubal closure is less than 60%.
Why is it difficult to determine the chance of tubal closure after Essure reversal?
To determine the exact chance of tubal closure after Essure, all patients who did not become pregnant after surgery would need to undergo a HSG x-ray to determine if the tubes are open or closed. Not only is this impractical, but HSG x-ray results are notoriously unreliable.
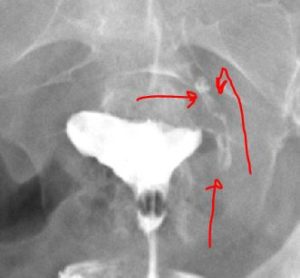
This HSG image after Essure reversal was incorrectly interpreted as both tubes being closed. The red arrows show dye passing the repair site and into the fallopian tube. The other side may be closed at the repair site or temporarily closed due to transient tubal spasm. HSG x-rays are not always accurate.
Many times these x-rays demonstrate tubal closure (dye does not enter the tubes) when, in fact, the tubes are really open but have a spasm (muscular tightening that will temporarily close the tubal opening) during the HSG x-ray.
It is not reasonable to have all Essure reversal patients have a follow-up HSG and the results of many of these x-rays would be unreliable.
Approximately 40% of patients will become pregnant after reversing Essure with Dr. Monteith.
Approximately 60% of patients will not become pregnant.
Those patients who do not become pregnant will have many reasons why pregnancy did not happen: (1) increased age, (2) other medical conditions, (3) male factors, and (4) tubal closure.
Tubal closure may be the most predominate reason why pregnancy does not happen for some patients after reversing Essure but it is difficult to determine the chance of tubal closure after Essure reversal with certainty.
Pregnancy Risks Of Reversing Essure: 5% Chance of Ectopic Pregnancy

Essure Reversal Baby from Dr Monteith
The main risk of any tubal ligation reversal surgery is the risk of ectopic (tubal) pregnancy.
When reversing tubal ligation types other than Essure, the risk of ectopic pregnancy ranges from 10% to 15%.
Dr. Monteith has observed the risk of ectopic pregnancy after Essure reversal seems to be lower than when reversing other types of tubal ligation.
Based on patient self-reporting, the risk of ectopic pregnancy after Essure reversal is approximately 5%.
Dr. Monteith has hypothesized the risk of ectopic pregnancy is lower in Essure reversal patients because Essure reversal either works or does not work… the fallopian tubes will either heal open or closed at the site of implantation.
- If Essure reversal works (one or both tubes heal open), the fertilized egg will make it into the uterus and will either be a normal pregnancy or an intrauterine pregnancy that will miscarry.
- If Essure reversal does not work (both tubes heal closed) pregnancy will not happen.
More information: Why does tubal reversal increase the risk of ectopic pregnancy?
Reversal of other tubal ligation procedures result in the tubes being repaired in the middle of the tube. The area where the repaired fallopian tubes are rejoined will always be an abnormal area where the fertilized egg may implant and develop within the fallopian tube.
Pregnancy Risks of Reversing Essure: Uterine Rupture 4%*
Essure causes blockage in the very beginning of the fallopian tube (the proximal portion of the fallopian tube).
The historical gold standard for surgically repairing fallopian tubes blocked in the location where the tubes insert into the uterus (proximal tubal blockage) is tubouterine implantation. This surgical procedure was first successful performed in the early 1900’s and more commonly in the mid-1900’s. There is a fair amount of medical literature highlighting the risk of uterine rupture after tubouterine implantation.
Four (4) patients experienced uterine rupture after Essure reversal. Most uterine ruptures were diagnosed between 36 to 38 weeks after patients complained of symptoms of uterine rupture; severe burning pain over the uterus in between contractions. In most cases, moms and the babies did well and without any major complications.
Patient #1. After 12 hours of painful contractions, she experienced gradually increasing abdominal pain at 36 weeks gestation. She underwent cesarean delivery and was diagnosed with a uterine rupture. The patient required blood transfusion; however, neither mom nor baby experienced a significant complication. This patient had a second pregnancy and underwent cesarean delivery without complication.
Patient #2. After reporting abdominal pain, she underwent emergency cesarean delivery and was diagnosed with uterine rupture at 36 weeks. Neither mom nor baby experienced a significant complication.
Patient #3. This patient was diagnosed with an asymptomatic uterine rupture during a scheduled cesarean delivery at 36 weeks. During the cesarean, her doctor discovered a 2 cm asymptomatic uterine window near one of the tubal implantation sites. Neither mom nor baby experienced a significant complication.
Patient #4. Her first pregnancy was delivered by scheduled cesarean delivery at 39 weeks without complication. During her second pregnancy, she experienced a uterine rupture at 37 weeks gestation, underwent an emergent cesarean delivery, and required a blood transfusion.
Her baby was admitted to the NICU, diagnosed with Hypoxic-Ischemic Encephalopathy, and underwent neonatal cooling therapy. The baby remained in intensive care for 3 weeks.
*Uterine Rupture Risk 4%. Dr. Monteith observed uterine ruptures in 4% of his patients who were pregnant after Essure reversal. Readers should be aware most patients underwent planned cesarean delivery. The 4% risk was observed in patients who did not make it to the date of their planned cesarean.
If all patients attempted vaginal delivery after Essure reversal, the observed risk of uterine rupture would likely be higher than 4%.
Risks of Reversing Essure: Why Does Dr. Monteith Recommend C-section?
 The uterus is similar to a latex balloon.
The uterus is similar to a latex balloon.
The non-pregnant uterus is like a balloon that has not been inflated. When pregnant and in the third trimester the uterus is like a maximally inflated balloon.
Essure reversal requires tubouterine implantation and each fallopian tube has to be reintroduced into the uterine muscle after the Essure devices have been removed. The areas on the uterine muscle where tubouterine reimplantation is performed will be a source of weakness for the uterine muscle.
Just like a balloon…when the uterine muscle is weakened and the uterus is maximally expanded there is a chance the uterus will tear (rupture) around the area of weakness.
Not only is the uterus like a balloon….but the uterus is a muscle and contracts during labor. The contractions will also cause extra stress to the weakened areas of the uterus.
Uterine rupture is not unique to Essure reversal surgery. The reason many doctors will recommend avoiding vaginal delivery after a previous cesarean is because of the risk of uterine rupture. Uterine ruptures can occur after cesarean delivery, fibroid removal surgery, or even from a weakened uterus after four (4) or more vaginal births.
Most uterine ruptures happen when in labor but can happen anytime during the third trimester of pregnancy.
Dr. Monteith’s professional recommendation is for his patients to have planned cesarean delivery (C-section) before going into labor with all future pregnancies after Essure reversal.

Dr Monteith of A Personal Choice
Dr. Monteith does not routinely record mode of delivery (vaginal birth vs cesarean).
As a result, he does not have statistics on how every Essure reversal patient delivered. Most of his Essure reversal patients followed his recommendations and underwent planned Cesarean delivery before going into labor.
Some patients had vaginal births (either planned or unexpected) without any complications.
Some Essure reversal doctor’s will advise their patients they can safely have a vaginal birth after reversing Essure. Unfortunately, these recommendations may be misleading.
Women considering Essure reversal with doctors who claim cesarean is not required should question the surgical techniques used by these doctors for reversing Essure. These alternative techniques and success rates of these alternative techniques have never been studied or published. In fact, many of these doctors have very few, if any, Essure reversal pregnancies.
Should a uterine rupture happen in (1) a patient who is unaware of this risk and (2) if the Essure reversal doctor has not discussed this unique risk with the patient’s primary doctor, an unexpected uterine rupture could have a catastrophic outcome for both mom and baby.

