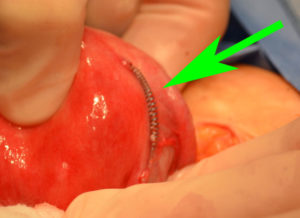
 We are frequently asked does health insurance pay for Essure removal?
We are frequently asked does health insurance pay for Essure removal?
Essure was first approved in 2001. At first not many women opted to have the Essure procedure. As doctors became more comfortable offering Essure and as the public became aware Essure was tubal ligation alternative, more women chose to use Essure for permanent birth control (sterilization).
Sterilization is intended to be permanent.
Research has shown that a significant number of women will regret their sterilization and desire to have another baby. Some of these women will consider in-vitro fertilization and some will consider surgical reversal of sterilization.
More info: Does health insurance pay for Essure reversal?
Some women get Essure and have abnormal side-effects. Many of these women will not want to become pregnant and only want the Essure devices removed. For these women they will need to choose between having a hysterectomy (removal of the uterus) or Essure removal (removal of the Essure devices only).
Essure reversal: Does Insurance Pay?
Essure reversal is a procedure to remove the Essure devices and reopen the fallopian tubes. The purpose of Essure reversal is to restore the natural function of the fallopian tube and allow for natural conception and pregnancy.
Health insurance companies consider Essure reversal and IVF as fertility treatments. They consider these procedures elective, non-urgent, or not life saving procedures. Essentially health insurance companies evaluate a patient’s request for Essure reversal the same way they would evaluate a patient’s request for a face lift or breast augmentation.
Fertility is not considered urgent or worthy of spending the companies money. Health insurance companies will never pay for Essure reversal.
Does health insurance pay for Essure removal?
A large number of women have reported abnormal side-effects after having the Essure devices inserted. Many of these women are having Essure devices removed, their fallopian tubes removed, or hysterectomy.
More information on Essure problems: Essure Problems Group Facebook Page
In the very beginning, both doctors and health insurance companies refused to acknowledge patients were having problems from Essure. The procedure to remove Essure was often not offered by doctors and declined by health insurance companies.
Over time as more patients have reported Essure complications, more doctors are willing to treat Essure problems and more health insurance companies have become willing to pay for treatment of Essure complications.
Does health insurance pay for Essure removal? Depends on the procedure
If you have been asking “Does health insurance pay for Essure removal?” The answer is yes….but only for certain removal procedure.
More information: Cost of Essure removal with Dr Monteith
Currently most health insurance companies will pay for Essure removal is you have a complete hysterectomy (removal of the uterus) or complete removal of the fallopian tubes along with the Essure devices. Health insurance companies will only pay for Essure removal if the hysterectomy or fallopian tube removal is done in a hospital setting.
If you want to become pregnant, health insurance companies will not pay for Essure reversal or in-vitro fertilization (IVF).
Does health insurance pay for Essure removal with Dr. Monteith?
 If you want Essure removed and want your insurance to pay for the entire procedure…then you will need to have your Essure devices removed in a hospital setting. You will either need to have a hysterectomy or removal of the fallopian tubes (total bilateral salpingectomy).
If you want Essure removed and want your insurance to pay for the entire procedure…then you will need to have your Essure devices removed in a hospital setting. You will either need to have a hysterectomy or removal of the fallopian tubes (total bilateral salpingectomy).
Dr. Monteith is a participating member in Blue Cross Blue Shield, Cigna, and Aetna and some of his Essure reversal and Essure removal patients are seeing partial reimbursement for Essure related surgery at A Personal Choice.
If you are a member of one of the above health insurance plans then you may be able to get reimbursement for Essure removal surgery with Dr. Monteith. Patients are required to pay in full before surgery. After surgery, A Personal Choice can submit your procedure to either Blue Cross, Cigna or Aetna to see if they will provide any reimbursements. Some patients have seen full reimbursement but most patients are seeing 0% to 20% coverage.