After Surgery Risks Of Removing Essure Devices
Essure removal With Dr Monteith: Analysis of 469 Patients
In January of 2018, Dr. Monteith performed an analysis on the risks of removing Essure devices at A Personal Choice.
From January of 2009 to January of 2018, Dr. Monteith performed 469 surgeries to remove Essure sterilization devices.
This group of 469 patients was comprised of women who requested Essure reversal (procedure to remove Essure and provide the chance of becoming pregnant) and also women who requested Essure removal (procedure to remove Essure devices for symptom treatment but prevents the chance of pregnancy).
To simply the discussion of risks of removing Essure devices, the following statistics will simply refer to Essure removal. This term will be used to include all patients who had surgery with Dr. Monteith (both Essure reversal and Essure removal patients).
The following postoperative complications were observed in the group of 469 patients who had Essure removal with Dr. Monteith.
Risks of Removing Essure Devices: Infections <1%
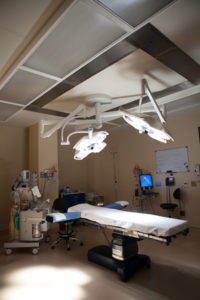 Major surgical site infections 0%
Major surgical site infections 0%
No major surgical infections occurred among patients undergoing Essure removal surgery with Dr. Monteith.
A major surgical site infection is infection which involves the pelvis, uterus, and fallopian tubes. The infection could be limited to the pelvis or could extend from the pelvis to the abdominal incision site.
Minor surgical site infections <1%
Two (2) patients were diagnosed with minor surgical site infections within the first month of surgery.
A minor surgical site infection involves the skin and underlying tissue. In both cases patients were evaluated and diagnosed by their local physicians and infections were treated with oral antibiotics and without any significant complications.
Risks of Removing Essure Devices: Needing Second Procedure within 30 Days <1%
Patient #1. Patient went to her local doctor four (4) days after Essure removal. She was experiencing abdominal pelvic pain. She was admitted to the hospital, underwent a diagnostic laparoscopy (camera inserted through the belly button), and blood was found within her pelvis and around her uterus. The blood was removed and she was discharged after overnight observation. She recovered without any additional complications.
Patient #2. After Essure removal surgery the patient returned home. Several days after her surgery, she began to experience abdominal pain and urinary changes. She was diagnosed with a hematoma (blood clot) underneath her incision and around the abdominal muscles. The hematoma was drained by an interventional radiologist by inserting a drainage catheter through the skin near the incision. She recovered without any additional complications.
Patient #3. After surgery the patient returned home and experienced persistent and worsening abdominal pain, bloating, nausea and vomiting. She presented to her local doctor and was diagnosed with an intestinal ileus (slow to return bowel function). She was observed after insertion of a nasogastric (NG) tube and her oral intake was limited. Her intestinal function recovered without the need for any additional treatment.
Patient #4. After surgery the patient returned home and experienced increasing abdominal pain three (3) days after Essure removal. She was evaluated in her local Emergency Room and diagnosed with an ileus (slow return of bowel function). She was discharged, continued to have pain, and returned for repeat evaluation approximately 5 days after her surgery. She was diagnosed with a hematoma (blood clot) behind the uterus and possible bowel obstruction. She was admitted, had a nasogastric (NG) tube inserted, underwent an exploratory laparotomy (abdominal incision) and was diagnosed with postoperative intra-abdominal bleeding after Essure removal and possible early small bowel obstruction.
Her recovery was delayed and she was hospitalized for approximately ten (10) days until her bowel function returned.
Persistent Symptoms Requiring Additional Surgery Estimated to be <10%
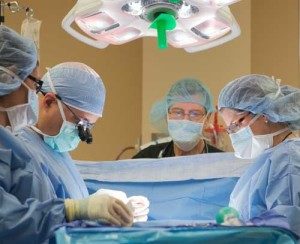 We estimate the risk of having persistent symptoms after removal of Essure requiring the need for additional surgery to be less than 10%.
We estimate the risk of having persistent symptoms after removal of Essure requiring the need for additional surgery to be less than 10%.
We don’t know the exact number of patients who may require additional surgery for Essure related symptoms. Why?
A significant number of our Essure removals are Essure reversals for patients who primarily desire to become pregnant and symptom treatment is often a secondary goal. If these patients have persistent symptoms after reversal, then many of them will delay additional surgery, if required, as they are attempting to achieve their pregnancy goals.
Occasionally additional surgery, if required, could be performed at any time over a patient’s life span. It is difficult to track patients far into the future. Moreover as other conditions develop it is challenging to know what required the need for an additional surgical procedure.
In 2014 we performed a survey study on 38 women who requested Essure removal for symptoms only. Of these patients 4% reported they required additional surgery to treat Essure related symptoms.
More info: Treating Essure symptoms: Essure removal study results
Postoperative Risks of Removing Essure Devices
The risks of removing Essure devices are low when having Essure removal with Dr. Monteith.
Infection
Major surgical infections after removal of Essure are rare.
Minor surgical infections are possible but the majority of these infections can be treated by the patient’s local doctor with antibiotics and, if needed, gauze packing of the incision.
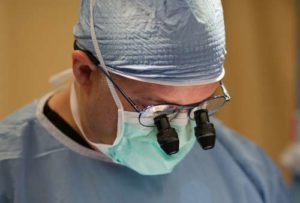 Dr. Monteith maintains a low rate of infection by: (1) having a specialty center dedicated to sterilization reversal (not the treatment of patients with a variety of medical conditions),
Dr. Monteith maintains a low rate of infection by: (1) having a specialty center dedicated to sterilization reversal (not the treatment of patients with a variety of medical conditions),
(2) limits the size of abdominal incisions and performs surgery in an efficient manner,
(3) has a skilled surgical staff and dedicated operating room allowing surgical times to be minimized,
(4) provides IV antibiotics during surgery to prevent infection,
(5) encourages patients to use Hibiclens surgical soap before and after surgery,
(6) encourages patients to follow-up with their local physicians after surgery, and
(7) maintains open lines of communication with patients to diagnose and treat surgical site infections.
Need for a second procedure within 30 days
Requiring a second procedure is a serious event but, thankfully, less than 1% of patients will require an additional procedure within 30 days of surgery with Dr. Monteith.
Bleeding after surgery and delayed return of bowel function are risks associated with any abdominal surgery and these risks cannot entirely be eliminated.
Surgical Complications: See No Evil, Hear No Evil, Speak No Evil
 No surgeon has a 0% complication rate. No procedure is 100% without risks.
No surgeon has a 0% complication rate. No procedure is 100% without risks.
All surgeons should strive to achieve a 0% complication rate but that level of perfection is not practical when taking care of a wide variety of patients.
If a surgeon reports never having had a complication and states they have a 100% safety record with a specific surgical procedure then these statements may not be entirely accurate.
These are the possible reasons why a surgeon may state they have never had a major surgical complication:
- Poor system of patient follow-up (see no evil)
- Poor system of patient communication (hear no evil)
- They are not being honest (speak no evil)
- They have done very few procedures
- They are extremely lucky
Many times not reporting surgical complications is a variation of the commonly heard phrase,
“Hear no evil, see no evil, speak no evil….”
There are no minor procedures and all procedures have risks.
