Essure tubal ligations are intended to be permanent, but we have perfected Essure reversal at A Personal Choice and can provide women the ability to become naturally pregnant again after Essure.
We were the first doctors in the world to publish successful reports of full term pregnancies after surgical reversal of both Essure and Adiana tubal ligation procedures.1-2
Essure: How Does It Work?
During an Essure procedure a small metal coil is placed inside the opening of each tube.
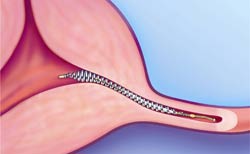 This causes the fallopian tube to heal closed by the formation of scar tissue inside the tube.
This causes the fallopian tube to heal closed by the formation of scar tissue inside the tube.
The scar tissue formation causes the fallopian tube to close from the inside but only in the very beginning of the tube.
The Essure coils are intended to permanently remain in the fallopian tubes after the scar tissue has formed.
Reversing Essure: We Were The First!
Dr. Charles Monteith and Dr. Gary Berger, the expert tubal reversal surgeons at A Personal Choice, published the first reports of successful reversal and pregnancy after both Adiana and Essure reversal in the peer reviewed medical literature. 1,2
These newer tubal ligation procedures are safely reversed at our specialty center through a 90 minute, outpatient operation called tubouterine implantation.
 Tubouterine implantation is the gold standard for the reversal of proximal tubal occlusion and tubal blockage from Essure.
Tubouterine implantation is the gold standard for the reversal of proximal tubal occlusion and tubal blockage from Essure.
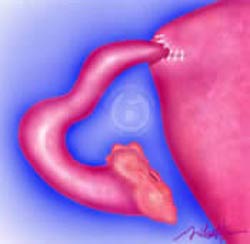
During a tubouterine implantation procedure, the healthy portion of each fallopian tube is separated from the uterus. The Essure coils are then removed to prevent complications with future pregnancies.
An incision is then made through the uterine muscle in a unscarred area of the uterus and the healthy portion of each tube is inserted into the uterine cavity. The uterine incision is then closed around the newly inserted tubes. The tubouterine implantation procedure is necessary to bypass the scarred portion of the fallopian tube caused by the Essure procedure.
Chances Of Pregnancy After Essure Reversal
We performed 90 Essure reversals between January 2009 and June 2013.
We allowed each patient 12 months of attempting pregnancy before including them in pregnancy success statistics. The 12 month follow-up has been completed on 56 patients and 16 of these patients have reported pregnancy.
The chance of pregnancy 12 months after Essure reversal surgery is 29%.
To view our updated and most current Essure reversal statistics: Reversing Essure Sterilization: Statistics Update.
Essure Reversal or IVF: Which Is Best?
The chance of pregnancy after in-vitro fertilization (IVF) is approximately 36%.3 The chance of pregnancy after Essure reversal at our center is 29%.
There is no data to suggest what the success rate of IVF is when the Essure coils are left in place. Several case reports do exist of successful IVF with Essure coils left in place.4,5
If the Essure coils project into the uterine cavity this may decrease the success of IVF. If the coils are left in place this may increase the risks of a pregnancy complication.
There are no good medical studies to suggest what the success rate of IVF is when the Essure coils have been left in place. There are no good medical studies on the risk of pregnancy with the Essure coils left in place.
Costs of Essure Reversal
The cost of Essure reversal is $7500 at our specialty center.
 This fee is all-inclusive and covers the pre-operative consultation, surgery to reverse Essure, anesthesia, and the postoperative recovery.
This fee is all-inclusive and covers the pre-operative consultation, surgery to reverse Essure, anesthesia, and the postoperative recovery.
In comparison, the average cost for a single IVF treatment cycle in the US is $12,000.
Most health insurances will not cover the cost of IVF or sterilization reversal. We offer a tubal reversal pre-payment option that allows patients to pay towards their reversal surgeries over time.
Is Essure Reversal Safe?
Tubouterine implantation can be safely performed as an outpatient procedure but may increase the risk of uterine rupture during labor.
Of the 90 Essure reversal surgeries we have performed, there have been no immediate surgical complications, no Essure reversal patient has reported an ectopic pregnancy, and no patient has reported a uterine rupture. One patient was seen by her doctor for abdominal pain 3 days after reversal surgery but otherwise had an uncomplicated post-operative course and a healthy, full term pregnancy.
None of our patients has had a complication from delivery after Essure reversal.
For maximal safety of both mother and baby, we advise our Essure reversal patients to have a scheduled cesarean delivery with future pregnancies to minimize the possible risk of uterine rupture. 6-8
More Information About Essure Reversal or Essure Removal
For more information about the cost of Essure reversal, please visit Tubal Reversal Cost.
If you have any questions about Essure reversal or Essure coil removal then please call and speak with one of our nurses for a free Essure reversal consultation (919) 968-4656.
Readers are also welcome to ask Dr. Monteith questions by submitting them through our Ask The Doctor section of our website.
References
1. Normal pregnancy after outpatient tubouterine implantation in patient with Adiana sterilization. Monteith CW, Berger GS. Fertility Sterility 2011;Jul 96(1) 45-6.
2. Successful Pregnancies After Removal of Intratubal Microinserts. Monteith CW, Berger GS. Obstet Gyncecol 2012;119:470-472.
3. 2010 Assisted Reproductive Technology Report. Centers for Disease Control and Prevention. 2010 National Report.
4. Successful pregnancy outcome with the use of in vitro fertilization after Essure hysteroscopic sterilization. Kerin JF, Cattanach S. Fertility Sterility 2007; May 87(5) 1212.
5. Essure multicenter off-label treatment for hydrosalpinx before in vitro fertilization. Galen DI, Khan N, Richter KS. J Minim Invasive Gynecol 2011; May-June;18(3):338-42.
6. Uterine rupture following tubal reimplantation. Review of the literature and report of three additional cases. Shortle B, Jewelewicz R. Obstet Gynecology Surv 1984 Jul;39(7):407-15.
7. Uterine rupture after tubal reimplantation. Horovitz J et al, J Gynecol Obstet Biol Reprod (Paris) 1988;17(5):650-2.
8. Uterine rupture after re-implantation of fallopian tubes. Brandt CA, Larsen B. Acta Obstet Gynecol Scand 1989;68(3):281-2.










