Tubal Ligation Syndrome
Can Tubal Ligation Cause Problems?
There are many articles on Post Tubal Ligation Syndrome within PubMed. Unfortunately most of these are poorly conducted medical studies. A full review of these articles will not be performed here. These studies suffer from poor design, small numbers, inadequate control groups, and inherent research bias. Moreover, Post Tubal Ligation Syndrome is reported to involve such a diverse range of varied symptoms that is it difficult to study adequately.
A discussion of Post Tubal Ligation Syndrome often becomes non-meaningful when an extensive list of adverse symptoms confronts a history of poor medical research. The more appropriate question may be can tubal ligation cause problems?
Can tubal ligation cause problems?
Some women do have problems after tubal ligation. Many of these problems are caused by easily identifiable causes (anovulation, endometriosis, adhesion formation, etc) but other symptoms have no easily identifiable cause and are either directly related to the tubal ligation or are coincidental. Many of our patients report improvement after tubal reversal surgery.
I have observed patients who have had problems caused directly by their tubal ligation. Often these women report improvement after reversal.
Menstrual Abnormalities and Tubal Ligation Syndrome: CREST Study
BACKGROUND: The existence of a post-tubal-ligation syndrome of menstrual abnormalities has been debated for decades. We used data from the U.S. Collaborative Review of Sterilization to determine whether the likelihood of persistent menstrual abnormalities was greater among women who had undergone tubal sterilization than among women who had not.
RESULTS: The women who had undergone sterilization were no more likely than those who had not undergone the procedure to report persistent changes in intermenstrual bleeding or the length of the menstrual cycle. They were more likely to have decreases in the number of days of bleeding (odds ratio, 2.4; 95 percent confidence interval, 1.1 to 5.2), the amount of bleeding (odds ratio, 1.5; 95 percent confidence interval, 1.1 to 2.0), and menstrual pain (odds ratio, 1.3; 95 percent confidence interval, 1.0 to 1.8) and to have an increase in cycle irregularity (odds ratio, 1.6; 95 percent confidence interval, 1.1 to 2.3). Among women who had had very heavy bleeding at base line, women who had undergone sterilization were more likely than women who had not undergone the procedure to report decreased bleeding (45 percent vs. 33 percent, P=0.03).
CONCLUSIONS: Women who have undergone tubal sterilization are no more likely than other women to have menstrual abnormalities.
The risk of menstrual abnormalities after tubal sterilization. U.S. Collaborative Review of Sterilization Working Group.
Peterson HB, Jeng G, Folger SG, Hillis SA, Marchbanks PA, Wilcox LS, U.S. Collaborative Review of Sterilization Working Group. N Engl J Med. 2000 Dec 7;343(23):1681.
Evidence for a post-tubal sterilization syndrome?
Tubal sterilization is not associated with an increased risk of menstrual dysfunction, dysmenorrhea, or increased premenstrual distress in women who undergo the procedure after age 30 years. There may be some increased risk for younger women, although they do not appear to undergo significant hormonal changes.
Is there any evidence for a post-tubal sterilization syndrome?
Gentile GP, Kaufman SC, Helbig DW. Fertil Steril. 1998 Feb;69(2):179.
Postablation-tubal sterilization syndrome
Operative resectoscopy and endometrial ablation are often performed to treat abnormal uterine bleeding, but little is known about the potential late complications of these procedures. We reviewed the records of 305 women who underwent endometrial ablation at a midwestern obstetrics and gynecology group practice and teaching hospital between July 1990 and October 1995. For 71 women, tubal ligation, salpingectomy, or tubal sterilization was performed at the time of ablation. Of these, six (8.4%) developed intense cyclic pain 5 to 40 months after surgery. Four subsequently underwent exploratory laparotomy and hysterectomy, and two others underwent laparoscopic tubal resection and destruction. Gross pathologic findings revealed hematosalpinx, and microscopic examination showed endometriosis, acute and chronic inflammation of the fallopian tubes, and acute and chronic myometritis. We believe these characteristic clinical and pathologic findings are consistent with postablation-tubal sterilization syndrome, a distinct clinical entity arising as a late complication of endometrial ablation in patients with a history of tubal ligations and/or obstruction.
Postablation-tubal sterilization syndrome. Postablation-tubal sterilization syndrome. Bae IH, Pagedas AC, Perkins HE, Bae DS. J Am Assoc Gynecol Laparosc. 1996 May;3(3):435.
Tubal ligation and Post Tubal Ligation Syndrome
The CREST study has been the gold standard for discussion regarding the existence of Post Tubal Ligation Syndrome. This is because this study was the first high quality, large cohort population study with an adequate control group. The CREST study firmly establishes women who have tubal ligation are not at increased risk for menstrual irregularities when compared to women who do not have tubal ligation. The CREST study provides a great example of how previous research suffered from inadequate controls and research bias.
Although the CREST study adequately evaluates for menstrual irregularities, the study does not fully address other symptoms some women report after tubal ligation.
Endometriosis explains some tubal ligation symptoms
I have personally been impressed how many patients I see who have endometriosis at the tubal ligation sites at the time of tubal reversal surgery.
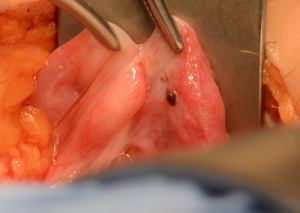 I commonly observe endometriosis during tubal surgery in uncommon locations: fallopian tube, tubal ligation sites, and in the broad ligament directly underneath the tubal ligation site. Often visible endometriosis will not exist in any other locations in these patients.
I commonly observe endometriosis during tubal surgery in uncommon locations: fallopian tube, tubal ligation sites, and in the broad ligament directly underneath the tubal ligation site. Often visible endometriosis will not exist in any other locations in these patients.
I have treated patients who have no prior history of endometriosis and no visible endometriosis at the time of tubal ligation who have subsequently developed symptoms after their tubal ligation.
Often these patients report dysmenorrhea or dyspareunia which evolved after their tubal ligation procedures. Many of these patients do not have a history of hormonal suppression which could masked symptoms before tubal ligation. On some occasions, as a result of their symptoms after tubal ligation, these patients have been diagnosed with depression, ovarian cysts, Irritable Bowel, Fibromyalgia, and other non-specific conditions.
I have also observed many of these same patients with endometriosis to be asymptomatic.

